Yves right here. This is a crucial put up, because it paperwork one more approach that the foundations of supposedly civilized life are eroding in America, right here entry to hospitals as a result of cash. And the headline is simply too charitable as to why that is occurring now. It’s not as a result of rural hospitals are all of a sudden seeing decay of their economics. It’s as a result of greater hospitals are shopping for them and shuttering them, presumably as a result of they consider they will power of us in these low-population areas to journey to see specialists and get surgical procedures. However what about emergencies? And what about those that are in hourly jobs and easily can’t take a half day or time without work simply to see a specialist, not to mention to get testing and care.
This text doesn’t incorporate the thought of personal fairness squeezing sufferers by shopping for up speciality follow like ER medical doctors and hospitalists, however I’ve to consider that performs a task.
Observe particularly the map of states with numerous rural hospitals at “quick danger” of closing. Ugly.
By run 75411. Initially printed at Angry Bear
That is an fascinating tackle small hospitals and likewise masking smaller hospitals in small cities or rural areas. It is a matter because the bigger hospitals purchase them up. Slightly than spend money on them, they shut them down. One reveal is these hospitals closings coming because of what non-public insurance coverage pays for affected person care.
This is a matter which each state and federal governments. needs to be addressing.
Why are 600+ rural hospitals vulnerable to closing? advisory.com. Commentary taken from:
“Rural Hospitals at Danger of Closing,” chqpr.org. Middle for Healthcare High quality and Fee Reform.
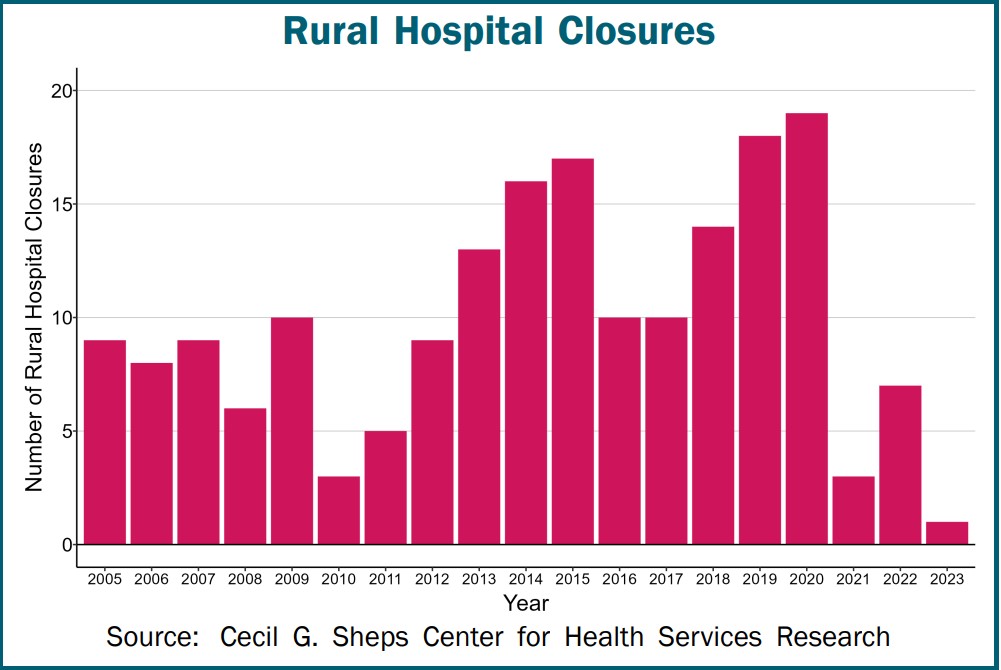
Issues are altering extra quickly. Smaller hospitals are below an assault of excessive prices and fewer income. Because of this, many are closing leaving the small city and rural residents with out medical care or having to drive lengthy distances in emergencies. As reported by Healthcare Quality and Payment Reform:
Many individuals throughout the nation couldn’t obtain hospital care of their neighborhood when the pandemic started. Over 150 rural hospitals closed between 2005 and 2019. A further 19 rural hospitals closed in 2020, greater than any yr within the earlier decade. The closures aren’t ensuing from the pandemic, however by monetary losses in earlier years. Ten extra rural hospitals closed in 2021 and 2022. The closures decreased in 2019 as a result of particular monetary help hospitals obtained in the course of the pandemic. The pandemic support has ended and closures are prone to improve.
Lots of of Hospitals are at Danger of Closing
600 rural hospitals or ~ 30% of all rural hospitals within the nation are vulnerable to closing. In danger due to the intense monetary issues, they’re experiencing:
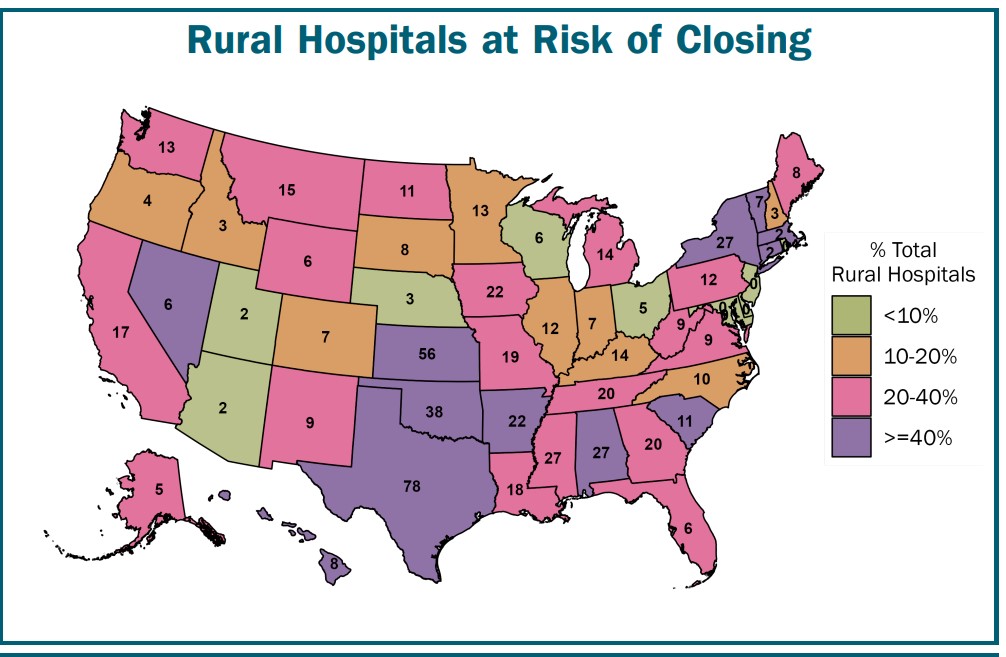
Losses on Affected person Companies: Medical health insurance plans aren’t paying these hospitals sufficient to cowl the price of delivering companies to sufferers. The losses will doubtless be higher sooner or later as a result of larger prices. All hospitals and notably small rural hospitals are experiencing such due to inflation and workforce shortages. Many of those hospitals have obtained grants, native tax revenues, or earnings from different actions offsetting losses on affected person companies prior to now. Nevertheless, there may be often no assure these funds will proceed to be accessible sooner or later or whether or not they are going to be enough to cowl prices.
Low Monetary Reserves: If the hospitals don’t obtain grants or different funds to cowl losses on companies, the hospitals wouldn’t have enough internet belongings (together with pandemic-related funding, however excluding buildings & tools) to offset their losses for greater than 6-7 years.
Many Rural Hospitals Are at Fast Danger of Closing
Over 200 of rural hospitals are at quick danger of closure. This as a result of severity of their monetary issues:
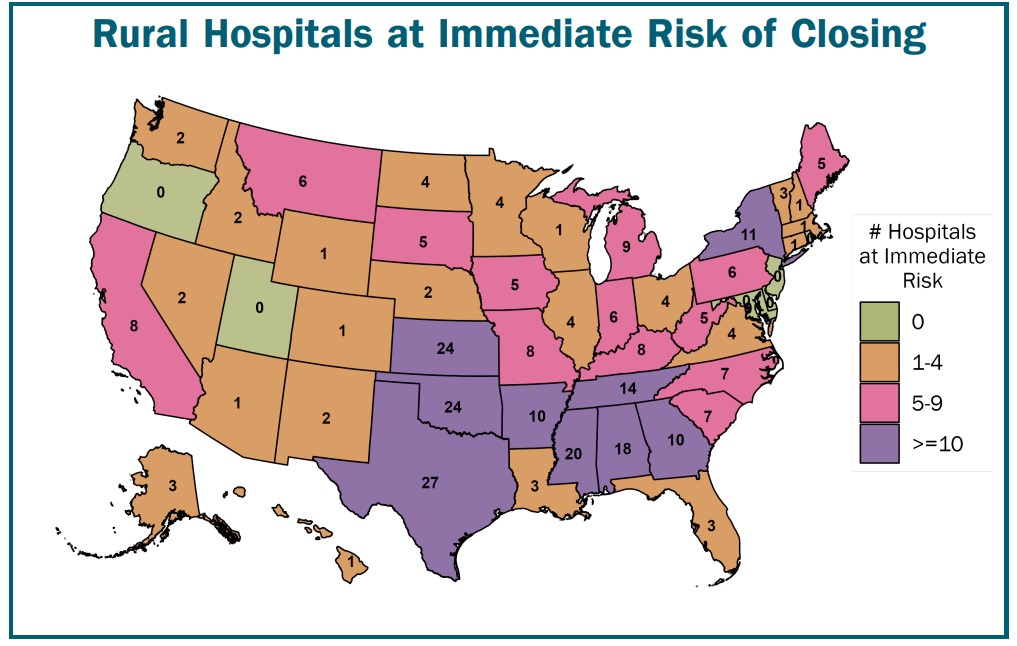
Insufficient Revenues to Cowl Bills: These hospitals misplaced cash delivering affected person companies over a multi-year interval (excluding the primary yr of the pandemic). They’re unlikely to obtain enough funds from different sources to cowl these losses after federal pandemic help ends.
Very Low Monetary Reserves: The hospitals have extra money owed than belongings, or the hospitals’ internet belongings (together with pandemic-related funding and excluding buildings & tools) might offset their losses for at an ~ 2-3 years. (Fewer rural hospitals are at quick danger than previous to the pandemic due to the federal pandemic support they obtained).
Entry Discount and growing Disparities for Rural
Many of the at-risk hospitals are positioned in remoted rural communities. Closure of the hospital would imply residents of the neighborhood would ravel a protracted distance for emergency or inpatient care. Additionally in lots of small rural communities, the hospital is the one place the place residents can get laboratory assessments or imaging research. It might be the one or principal supply of main care locally. A closure of the hospital would trigger a lack of entry to many important healthcare companies.
What I like about this text is it including a distinct viewpoint of why small hospitals are in monetary bother is the following portion of the article. The subsequent two subjects come as a shocker.
Closures Are Brought on by Insufficient Funds from Personal Payers
The first cause a whole bunch of rural hospitals vulnerable to closing is non-public insurance coverage are paying them lower than what it prices to ship companies to sufferers. As proven, though the at-risk hospitals are dropping cash on uninsured sufferers and Medicaid sufferers . . . losses on non-public insurance coverage sufferers are the most important reason behind their general losses.
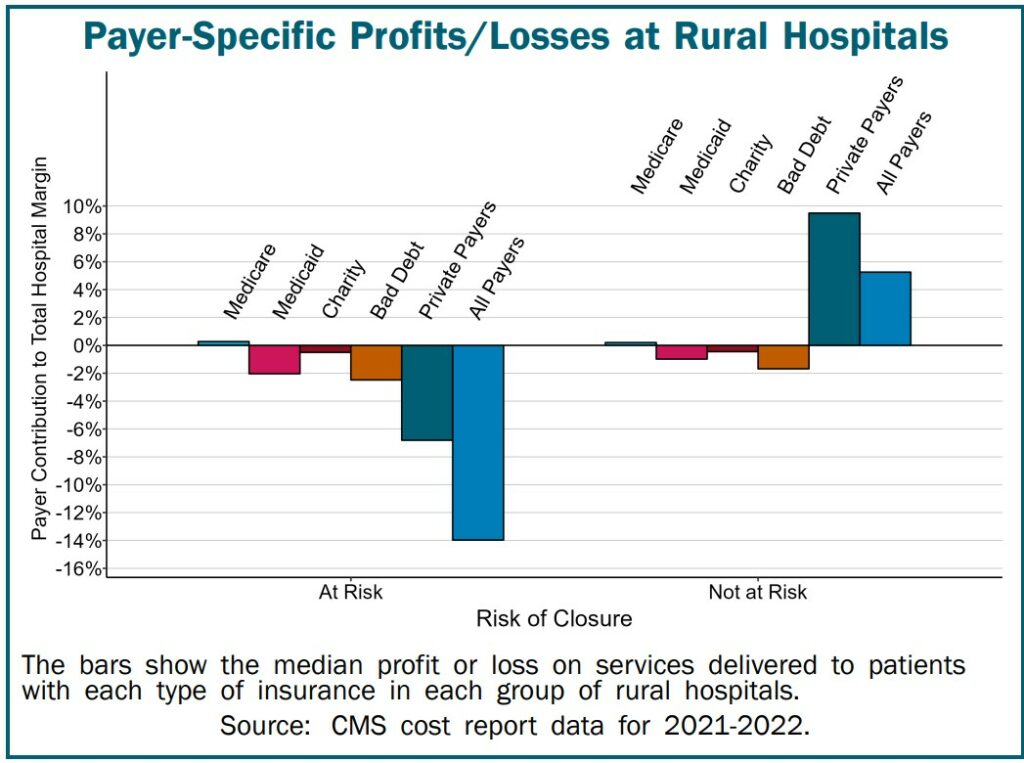
Conversely, many rural hospitals not vulnerable to closing as a result of they make earnings on affected person companies. They obtain funds from non-public well being plans masking the prices of delivering companies to the sufferers with non-public insurance coverage. These funds additionally offset the hospitals’ losses on companies delivered to uninsured and Medicaid sufferers.
Observe: Medicare is just not one of many causes placing rural or small hospitals in danger.
Stopping Rural Hospital Closures
Modifications are being referred to as for in each the quantities and technique of cost for rural hospital companies to be able to forestall extra rural hospitals from closing sooner or later. Rural hospital closures threaten the nation’s meals provide and vitality manufacturing. The reasoning are the finding of Farms, ranches, mines, drilling websites, wind farms, and photo voltaic vitality amenities are positioned primarily in rural areas. They won’t be able to draw and retain staff if the employees can’t get enough healthcare companies.
Requiring Healthcare Companies to Cowl the Price of Companies in Rural Communities
Funds which might be enough to cowl the price of companies at massive hospitals is not going to be enough at small rural hospitals as a result of it prices extra to ship healthcare companies in rural communities. This isn’t as a result of rural hospitals are inefficient, however due to the smaller variety of sufferers served relative to the mounted prices of the companies. For instance, a small rural neighborhood may have fewer Emergency Division (ED) visits than a bigger neighborhood just because there are fewer residents, however the minimal price of staffing the ED on a 24/7 foundation would be the identical, so the common price per go to will likely be larger.
The largest drawback going through small rural hospitals is insufficient funds from non-public well being plans. Most “options” for rural hospitals have targeted on growing Medicare or Medicaid funds or increasing Medicaid eligibility on account of a mistaken perception most rural sufferers are insured by Medicare and Medicaid or are uninsured.
In actuality, about half of the companies on the common rural hospital are delivered to sufferers with non-public insurance coverage (employer-sponsored insurance coverage and Medicare Benefit plans). Most often, the quantities these non-public plans pay, not Medicare or Medicaid funds, decide whether or not a rural hospital should shut.
Rural hospitals shouldn’t be pressured to get rid of inpatient care to be able to obtain larger funds for different companies, as is required below the federal “Rural Emergency Hospital” program. This might make it tougher for rural residents, notably the aged, to obtain immediate, high-quality care when they’re ailing.
Rising funds to ranges enough to stop closures of the at-risk hospitals would price about $4 billion per yr. This might signify a rise of just one/10 of 1% in complete nationwide healthcare spending. Many of the larger spending would help main care and emergency care, because the largest causes of losses at most small rural hospitals are underpayments for main care and emergency companies. Spending would doubtless improve as a lot or greater than this if hospitals shut, as a result of lowered entry to preventive care and failure to obtain immediate therapy will trigger residents of the communities to be sicker and want extra service sooner or later.
Create Standby Capability Funds to Help the Fastened Prices of Important Rural Companies
The monetary issues at small rural hospitals are prompted not solely by the insufficient quantities paid by non-public medical health insurance and Medicaid plans, however by the problematic technique all payers use to pay for companies. Small rural hospitals aren’t paid in any respect for what residents of a rural neighborhood would doubtless view as one of the necessary companies of all – the supply of physicians, nurses, and different workers to deal with an harm or critical well being drawback shortly if the resident experiences an harm or drawback. Having medical health insurance that pays charges for ED visits, laboratory assessments, or therapies is of little worth if there isn’t a Emergency Division, laboratory, or therapy functionality accessible locally for the resident to make use of.
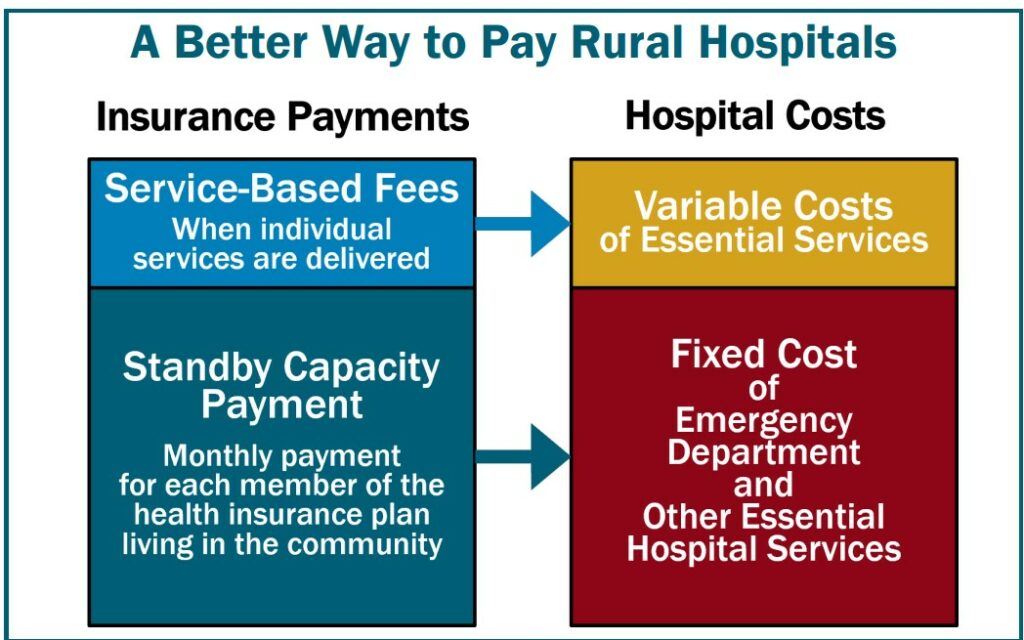
To be able to protect and strengthen important hospital companies in rural communities, small rural hospitals have to obtain Standby Capability Funds from each non-public and public payers along with being paid Service-Primarily based Charges when particular person companies are delivered. The Standby Capability Fee would help the mounted prices of important companies on the hospital, and the Service-Primarily based Charges would cowl the variable prices of these companies.
Extra particulars on this strategy can be found in A Better Way to Fund Rural Hospitals.









